News
Powerful short film from Future Fertility uniquely captures the emotional journey of fertility treatment

The path to parenthood isn’t always as straightforward as one hopes.
A new short film, “The Other Mothers”, created by fertility AI pioneer Future Fertility and digital marketing agency WeThink Nordic, aims to profile the emotional perspectives of patients going through fertility treatments.
“The Other Mothers” builds upon the already growing social movement around patients coming forward to speak out about their experiences, hardships, successes, and failures, helping to normalise discussions about the challenges that hopeful parents endure on their quest to conceive.
WeThink’s concept was guided by a voiceover script penned by a writer who had gone through her own intense fertility, leading to her first child.
Almost by fate, the woman who recorded the spoken voiceover had also undergone IVF treatments and recognised those same feelings reflected in the script.
“Echoing the many posts we’d dug through on online forums, we were touched by the wide range of emotions that such a difficult period brings on and knew that our film had to capture that reality as best as it could,” says Thomas Bo Nielsen, WeThink Nordic’s Creative Director.
“We felt extremely grateful that we were able to materialise our creative concept in a way that’s undoubtedly authentic – which is super important to us when covering a topic that resonates so strongly with a large number of people across the world.”
“Undergoing fertility treatment, whether it’s IVF or egg freezing, is so emotionally and physically taxing, and so many patients carry the mental burden of it alone,” adds Ghita Holst, Partner at WeThink Nordic.
“They often feel uncomfortable about opening up about their experience because it still seems like a taboo subject to talk about in many social circles.”
The film pushes this narrative front and centre, grounding the audience in the emotional pressure experienced by patients undergoing the fertility process and the common feeling that they need to portray a positive disposition for the benefit of others.
“Two pink lines isn’t something we just get.
“We get the uncertainty, the anxiety, the experimenting, the pretending that we’re ‘okay’…that we’re so happy for the women whose path to parenthood turned out differently.”
Beyond the messaging, what makes the film even more impactful is the realism brought to the story via images of actual patients (featuring family, friends, and employees who have gone through the process).
This is strengthened by the participation of Future Fertility’s partner clinics worldwide, who support real patients with these challenges every day.
“There was an incredible sense of community in producing this video,” said Kirsten Anwender, Future Fertility’s Director of Marketing.
“We’re grateful to our patient contributors, who were so generous in entrusting us to share their deeply personal stories with the world.
“Our clinic partners also instantly connected with our vision and were excited to take part. WeThink developed a great concept that truly struck a chord with everyone.”
For fertility patients who were invited to preview the film, the message certainly hit home.
“It’s a really powerful video,” says Heather, one of the film’s IVF patient contributors.
“The first time I saw the final cut, I had to watch it a few times in a row and let the emotions just roll over me.
“It can be so hard to look back at that time because you feel so alone and scared. It was nice to see my experience mirrored and narrated with such care.”
“Like many couples, we didn’t know we would have difficulty conceiving until we tried,” comments Mamiko, another IVF patient who was featured.
“The video captures the overwhelming feeling of uncertainty that impacted many aspects of our lives.”
Two-time IVF mum Ayla reflects: “To me, the video really illustrates the loss of the care-free aspects of conception, the loss of the pleasant “surprise”.
“How you resent having to rely on the science but are also in awe of it and grateful for it.
“How, when you’re lucky enough to end up with a baby in your arms, the differences and discomforts of your journey to get there fade into the background again.”
“The Other Mothers” leaves the audience with a closing message of hope, highlighting the advancements in fertility science and technology that are continuing to improve outcomes and access.
It also honours the tireless, amazing embryologists, providers and clinicians that work diligently to achieve results for their patients.
Future Fertility has been working to close the gaps in fertility science as the first company to provide personalised egg quality assessments for egg freezing and IVF patients, leveraging the power of artificial intelligence to analyse images of each individual egg.
“Being patient-centred is very important in fertility care, and as a whole, the industry has quite a long way to go to achieve this fully,” says Nicole Condon, CEO of TRIO Fertility and Founder of EVOLVE Egg Freezing Clinic – both clinics being early adopters of Future Fertility’s technology.
“Patients deserve to be at the centre of their care, and tools like this enable clinics to empower patients with personalised insights so they can be more informed and more engaged in their treatment decisions.”
As the demand for egg freezing and IVF treatments continues to grow globally, advancements in fertility technology can assist clinics in optimising treatments through precision medicine and providing patients with greater access to care by making fertility journeys more efficient.

Pregnancy
Physicians neglecting preventive care for women with diabetes, study finds
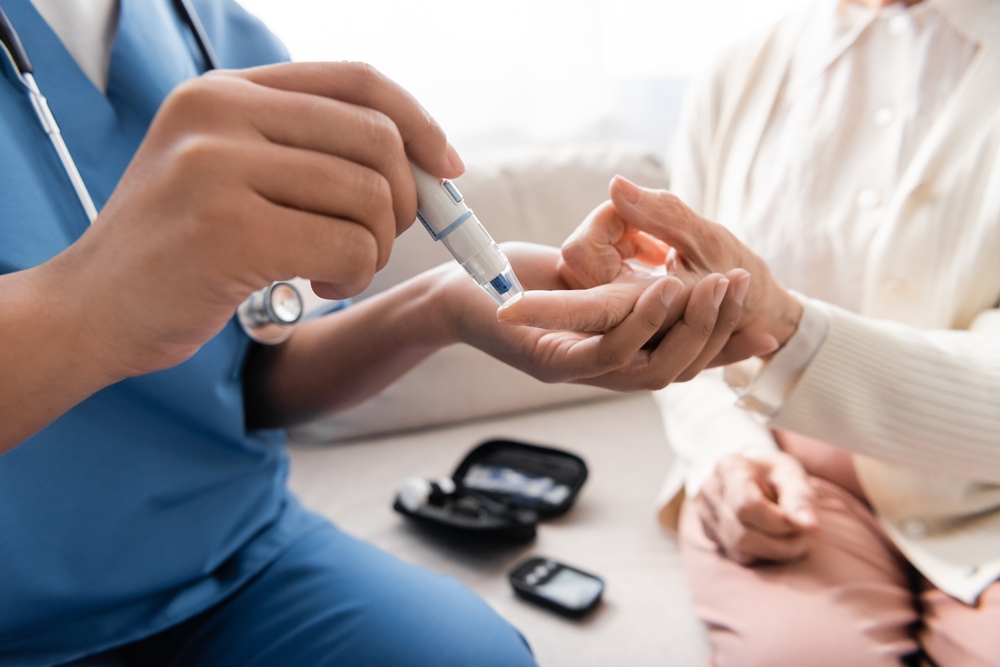
Women with diabetes are less likely to get preventive care than those without the condition, a UCLA-led study suggests.
The findings are based on an analysis of more than 40 studies from several countries.
They highlight how physicians largely overlook the importance of these routine services for women who have diabetes mellitus, or DM, putting them at risk of preventable medical conditions such as pregnancy complications.
Lauren Wisk is associate professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA and senior author on the study.
She said: “These findings are important because they identify that women with diabetes are not receiving recommended well-woman care, which is essential to support both managing their diabetes and their overall health.
“Providers need to be aware that they should not forget to provide these essential services for women with diabetes.”
The researchers sifted through thousands of studies, focusing on the concepts of women, diabetes and women’s health services, and settled on 44 that addressed treatment services for women aged 15 to 49 with type 1 or type 2 diabetes, excluding those with diabetes insipidus or gestational diabetes.
They looked at four preventive health service categories: contraceptive counselling and use, breast and cervical cancer screening, pre-conception counselling, and screening for sexually transmitted infections.
One study found that 48 per cent of women with diabetes received contraceptive services compared with 62 per cent of women without the disease.
Nine papers showed cervical cancer screening rates ranging from 38 to 79 per cent for women with diabetes compared with 46 to 86 per cent for those without diabetes.
Four studies found that breast cancer screening rates for women with diabetes ranged between 38 and 69 per cent compared with 54 and 82 per cent for those without diabetes.
Fourteen studies found pre-conception counselling rates of just over 1 per cent compared with 46 per cent for women with diabetes who are planning to get pregnant.
The researchers did not identify any studies on screening for sexually transmitted infections, which they said represents “a substantial gap in the literature.”
The researchers wrote: “One of the more striking findings of this review is the importance of robust coordinated care teams in ensuring access to appropriate services for women with DM.
“Several of the identified studies provide support that a co-management model, or the concept of involving endocrinology, primary care, and other specialty care providers in the care of individuals with DM, as recommended by the American Diabetes Association, is associated with greater receipt of services.”
Within the time constraints of an office visit, primary care physicians are expected to address preventative health needs as well as chronic disease management, said Dr Lisa Kransdorf, an associate clinical professor of medicine at the Geffen School and a study co-author.
She said chronic disease management will often take priority.
“In cases where the patient has other providers such as specialists and clinical pharmacists actively involved in their chronic disease management, there is opportunity for primary care physicians to attend to preventative care gaps,” the researcher added:
There are some limitations to the findings.
The search yielded only 44 studies, many of which relied on patient recall, which can be unreliable, highlighting the need for further research.
In addition, most of the studies analysed had small sample sizes or were conducted at a single site, limiting how applicable the findings might be in other settings.
Wellness
WUKA’s Tackle Anything campaign reaches 6,000 Girls

WUKA’s Tackle Anything campaign has officially reached their goal of supporting 6,000 girls across grassroots sports clubs in the UK – making a major milestone in the fight to keep girls in sport.
WUKA believes no girl should have to stop playing because of her period.
Yet for many young athletes, that’s still the reality. Fear of leaking through kit, managing cramps during training, or lacking access to sustainable period products continues to push girls out of sport.
The scale of the issue is impossible to ignore:
- 3 in 4 girls avoid sport and physical activity during their period
- This figure rises to 78 per cent among girls who have dropped out of sports.
- 43 per cent of girls drop out of sport after primary school
Source: https://womeninsport.org
That’s why WUKA, the award-winning, pioneering, female-founded period care brand, launched Tackle Anything – a campaign designed to support girls at grassroots level and create more period-inclusive sports environments from the very start of their journeys.
Since launching, the initiative has supported over 6,000 girls across a wide range of sports, including football, rugby, netball, roller hockey and taekwondo, reaching clubs in England, Scotland and Wales.
Through the campaign, clubs receive free WUKA Teen Stretch period underwear for young athletes, alongside expert-led period education delivered in partnership with 3x Olympian and Commonwealth, Euro & World Champion Hannah Miley MBE.
The programme helps coaches, parents and players feel more confident supporting girls in sport – both physically and emotionally
Continuing the Mission
While reaching 6,000 girls is a huge milestone, WUKA says the work is far from over.
The brand is continuing to expand Tackle Anything, with plans to support even more clubs and reach thousands more girls – ensuring that periods are no longer a barrier to participation in sport.
Because staying in the game shouldn’t depend on your cycle.
Founder and CEO of WUKA, Ruby Raut says: “At WUKA, this has never been about visibility – it’s about freedom.
“Freedom for girls to show up, play, and stay in sport without their period holding them back. Reaching 6,000 girls is a huge milestone, but for us, it’s part of a much bigger fight.
“We’ve already helped change the game, and we’re committed to continuing that progress.
“Every time we hit a goal, we set a new one — because this isn’t the finish line. It’s about shaping the future of sport and making sure the next generation grows up feeling confident, supported, and unstoppable.
Dean Wigzell (Head of Community Engagement at Kings Langley FC) adds: “The club is proud to be working with WUKA.
“Partnerships like this further reinforce our belief that our club is fast becoming the club to be at for young female footballers.”
The WUKA Mission:
WUKA – short for Wake Up Kick Ass – is on a mission to eliminate shame, silence, and stigma around periods.
Their commitment to menstrual equity in sport is starting where it matters most: at the beginning.
Because when you empower girls early, you don’t just keep them in the game – you change the future of the game itself.
Part of a Bigger Fight
This builds on WUKA’s wider activism – including their #AxeTheTax campaign, which successfully removed the tax on period pants, and continues to fight for true menstrual equity in the UK, including in sports.
Because access isn’t a luxury – it’s a right. WUKA is now making sure girls aren’t priced out of the game or made to feel like their period holds them back.
This isn’t just about products – it’s about freedom, fairness, and creating a level playing field for every girl.
To learn more about the campaign or explore how your club or organisation can get involved, visit: https://wuka.co.uk/pages/tackle-anything.
Fertility
NICE issues fertility guidance for people with endometriosis

NICE has updated fertility guidance with a new endometriosis section for people struggling to conceive.
This follows feedback received during public consultation, recognising for the first time that the condition requires its own tailored approach to fertility care, separate from other causes of infertility.
Emma Cox, chief executive of Endometriosis UK, said: “This year’s Endometriosis Action Month theme is ‘Endometriosis Doesn’t Wait’ and our new State of Endometriosis Care report shows just how urgently change is needed.
“With average diagnosis times now standing at 9 years and 4 months, and 11 years for those from ethnically diverse communities, many have already waited far too long by the time they reach fertility services.
Today’s guidance marks a step change in the fertility support that anyone with endometriosis should receive.
“For years, those with endometriosis have told us they felt invisible within the fertility system, grouped with unexplained infertility despite having a diagnosed condition.
“We welcome NICE’s decision to listen to patient voices during consultation, to create a dedicated pathway, and to remove misleading labels like ‘mild’ and ‘severe’ endometriosis.”
“Endometriosis doesn’t wait. And now, at last, neither will the guidance.”
Endometriosis UK and others told NICE during consultation that endometriosis was being grouped with unexplained infertility, despite it being a diagnosed condition.
The committee agreed this was inappropriate and that endometriosis requires a distinct fertility pathway.
Respondents also told NICE that terms such as “mild” and “severe” endometriosis were clinically ambiguous and did not reflect the complexity of the condition or its impact on fertility.
The committee agreed and those terms have been removed from the final guideline.
Under the new recommendations, clinicians will discuss a range of options with patients with endometriosis who are trying to conceive, taking into account individual factors including how long they have been trying to conceive, the severity of their symptoms, their age, their ovarian reserve, which is a measure of remaining egg supply, and any male fertility factors.
The guideline sets out a treatment pathway. Where appropriate, expectant management, meaning time to try to conceive naturally, may be offered, or surgical treatment to address endometriosis, in line with NICE’s existing endometriosis guideline (NG73).
If neither approach is suitable or successful after 2 years, fertility treatment options including intrauterine insemination (IUI), where sperm is placed directly into the womb, or IVF will be discussed.
The new guidance supports the ambitions set out in the NHS 10 Year Health Plan, which commits to shifting care closer to home and empowering patients and professionals to make the best choices about treatment.
Setting out a clear, personalised pathway in the guideline for endometriosis helps ensure fertility services are better tailored to individual need, reducing variation in care and supporting equitable access across England.
Eric Power, interim director of the Centre for Guidelines at NICE, said: “We listened carefully to what patients, clinicians and patient groups told us during consultation.
“They described how complex endometriosis is, how they felt existing labels were misleading, and that the condition needed its own pathway. The committee agreed and acted on that feedback.”
“By creating a dedicated section for endometriosis, we are giving clinicians a clear, evidence-based framework to have better, more personalised conversations with their patients, ensuring that everyone, regardless of the cause of their fertility problems, has access to the right care at the right time.”
Public health minister Sharon Hodgson said: “Every woman with endometriosis deserves fertility care that recognises the complexity of her condition.
“This landmark guidance will ensure women can access a clear, personalised pathway to fertility care that leads to clearer conversations with clinicians and fewer barriers.
“We’re committed to giving every woman the support she deserves, and today’s guidance is a significant step towards ending the inconsistency that has let down too many, for too long.”

 Diagnosis4 weeks ago
Diagnosis4 weeks agoBlood test shows promise in endometriosis

 Insight4 weeks ago
Insight4 weeks agoWomen’s health leaders warn of censorship

 Insight4 weeks ago
Insight4 weeks agoBlood test predicts dementia 25 years before symptoms begin

 Menopause4 weeks ago
Menopause4 weeks agoStudy reveals hidden menopause tech privacy concerns

 News3 weeks ago
News3 weeks agoFemtech World Awards announces deadline extension

 News3 weeks ago
News3 weeks agoLuna and Kindbody partner to bring data-driven insight to women’s health and fertility care

 News4 weeks ago
News4 weeks agoPregnancy may shed brain’s grey matter to prepare women for motherhood – study

 Menopause4 weeks ago
Menopause4 weeks agoNon-hormonal menopause pill approved for NHS use

























2 Comments